HAVE YOUR SAY.
Join us in The Bullpen, where the members of the Scientific Inquirer community get to shape the site’s editorial decision making. We’ll be discussing people and companies to profile on the site. On Wednesday, August 3 at 5:30pm EST, join us on Discord and let’s build the best Scientific Inquirer possible.
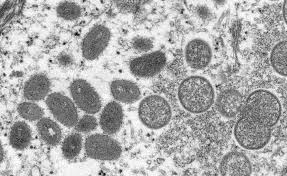
A study published by The BMJ today identifies important differences in monkeypox symptoms between the current outbreak and previous outbreaks in endemic regions.
The findings are based on 197 confirmed monkeypox cases at an infectious disease centre in London between May and July 2022.
Some of the common symptoms they describe, including rectal pain and penile swelling (oedema), differ from those described in previous outbreaks.

As such, the researchers recommend that clinicians consider monkeypox infection in patients presenting with these symptoms. And they say those with confirmed monkeypox infection with extensive penile lesions or severe rectal pain “should be considered for ongoing review or inpatient management.”
According to government data, as of 18 July 2022, there were 2,137 confirmed cases of monkeypox in the UK. Of these, 2,050 were in England and almost three quarters (73%) were in London.
All 197 participants in this study were men (average age 38 years), of whom 196 identified as gay, bisexual, or other men who have sex with men.
All patients presented with lesions on their skin or mucosal membranes, most commonly on the genitals or in the perianal area.
Most (86%) of patients reported systemic illness (affecting the entire body). The most common systemic symptoms were fever (62%), swollen lymph nodes (58%), and muscle aches and pain (32%).
And in contrast with existing case reports suggesting that systemic symptoms precede skin lesions, 38% of patients developed systemic symptoms after the onset of mucocutaneous lesions, while 14% presented with lesions without systemic features.
A total of 71 patients reported rectal pain, 33 sore throat, and 31 penile oedema, while 27 had oral lesions, 22 had a solitary lesion, and 9 had swollen tonsils.
The authors note that solitary lesions and swollen tonsils were not previously known to be typical features of monkeypox infection, and could be mistaken for other conditions.
Just over a third (36%) of participants also had HIV infection and 32% of those screened for sexually transmitted infections had a sexually transmitted infection.
Overall, 20 (10%) of participants were admitted to hospital for the management of symptoms, most commonly rectal pain and penile swelling. However, no deaths were reported and no patients required intensive hospital care.
Only one participant had recently travelled to an endemic region, confirming ongoing transmission within the UK, and only a quarter of patients had known contact with someone with confirmed monkeypox infection, raising the possibility of transmission by people with no or very few symptoms.
The authors acknowledge some limitations, such as the observational nature of the findings, the potential variability of clinical record keeping, and the fact that the data are limited to a single centre.
However, they say these findings confirm the ongoing unprecedented community transmission of monkeypox virus among gay, bisexual, and other men who have sex with men seen in the UK and many other non-endemic countries.
They write: “Understanding these findings will have major implications for contact tracing, public health advice, and ongoing infection control and isolation measures.”
And they call for continued research to inform infection control and isolation policies and guide the development of new diagnostics, treatments, and preventive measures.
IMAGE CREDIT: NIH.




Leave a Reply