Ann Arbor, December 15, 2021 – A study of the impact of national face mask laws on COVID-19 mortality in 44 countries with a combined population of nearly one billion people found that, over time, the increase in COVID-19 related deaths was significantly slower in countries that imposed mask laws compared to countries that did not. The study, appearing in the American Journal of Preventive Medicine, published by Elsevier, shows that masks provide a supplementary layer of protection that could prevent unnecessary COVID-19 deaths.
“While several studies before this have looked at the impact of masks on COVID-19 cases, fewer studies were focused on whether mask wearing may reduce COVID-19 deaths, and no study had looked at the data across multiple countries,” said lead investigator Sahar Motallebi, MD, MPH, from Malmo, Sweden. “The large sample of culturally diverse countries in this retrospective study covers a large population, giving us more evidence towards the life-saving potential of masks during the COVID-19 pandemic.”
The top 50 countries according to the United Nations Development Programme Human Development Index, which measures life expectancy, education, and standard of living, were targeted because of comparability and reduced chance of selection bias. Four countries in the Southern Hemisphere (New Zealand, Australia, Chile, and Argentina) were excluded to avoid potential seasonality characteristics. The United States and Canada were excluded because public health policies are made at the state/province level and a unified national policy does not exist. Data from the remaining 44 countries were used to model COVID-19 mortality.
Twenty-seven countries with face mask policies and 17 countries without face mask policies, covering a combined population of nearly one billion people, were included in the study. Investigators looked at COVID-19 deaths between February 15, 2020, the date of the first confirmed death in the targeted countries, to May 31, 2020, when many countries began to lift gathering and movement restrictions. Ten relevant demographic, social, clinical and time-dependent factors were examined. Potential confounders between face mask policy and mortality reduction, such as non-pharmaceutical interventions, were identified.
The 44 countries studied reported 2,167,664 confirmed deaths, 1,253,757 in countries without face mask mandates and 913,907 in countries with face mask mandates. The average COVID-19 mortality per million population was 48.40 in countries with face mask policies and 288.54 in countries without face mask policies, and this was significantly greater compared to countries with mask mandates. Face mask countries had significantly lower average daily increase in deaths compared to no face mask countries.
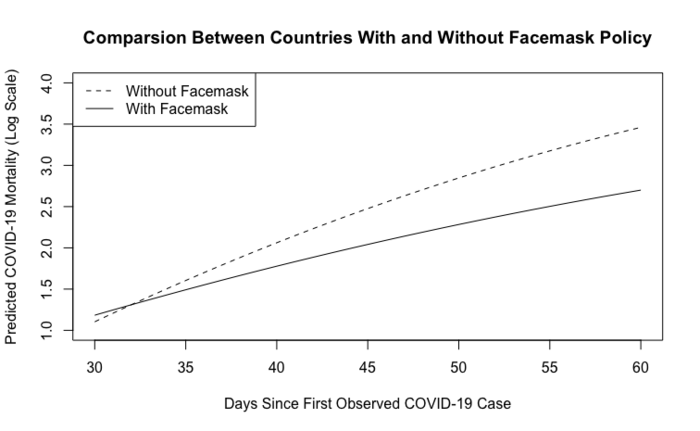
Surprisingly, the countries with no mask mandate started with a lower COVID-19 daily mortality. However, the death rate accelerated so fast in those countries that they not only caught up with the death rate in mask law countries, but significantly surpassed them over time.
“To reach its full potential of saving lives, public health research should be practical and pragmatic,” Dr. Motallebi stressed. “Our primary objective was to assess lessons learned from the pandemic in order to better prepare for future potential epidemics of airborne diseases, before pharmaceutical interventions are available.”
As delays in vaccination continue to challenge heath systems across the globe, the study adds evidence that before, and even after, full vaccination of the population, face masks continue to be a preventive measure against COVID-19.
“Across variants, vaccines may reduce mortality but not necessarily morbidity, and face masks continue to protect against both. So, we don’t have to choose between these two good policies of vaccination and face masks or substitute one for the other when we can and must do both in parallel,” Dr. Motallebi concluded.
IMAGE CREDIT: American Journal of Preventive Medicine




Leave a Reply