A collaboration between UK, Canadian and Chinese scientists has helped to reduce the over-prescription of unneeded antibiotics to children in rural China, according to research published today in Lancet Global Health.
Children in some areas of the country are being given antibiotics, often intravenously, to treat a cold, ear or throat infections, but the drugs are not effective against virus based illnesses.
The inappropriate use of antibiotics is a major risk factor in the development of drug-resistant ‘superbugs’.
A project designed by the scientists to curb the prescribing of antibiotics for children with upper respiratory tract infections saw antibiotic use drop by half.
The collaboration brought together rural hospitals in two counties in rural China, Chinese health officials and academics at the University of Leeds and University of Toronto.
The aim was to devise and evaluate a system of ‘anti-microbial stewardship’ that could be used in other parts of the Chinese health system and would give doctors the confidence to say ‘no’ to requests for inappropriate antibiotic treatment.
The stewardship programme was rolled out to a group of primary care rural hospitals in in Guangxi province in Southern China. A lot of demand for antibiotics in the Chinese primary care sector comes from parents and grandparents who have children with upper respiratory tract infections such as a sore throat or ear ache.
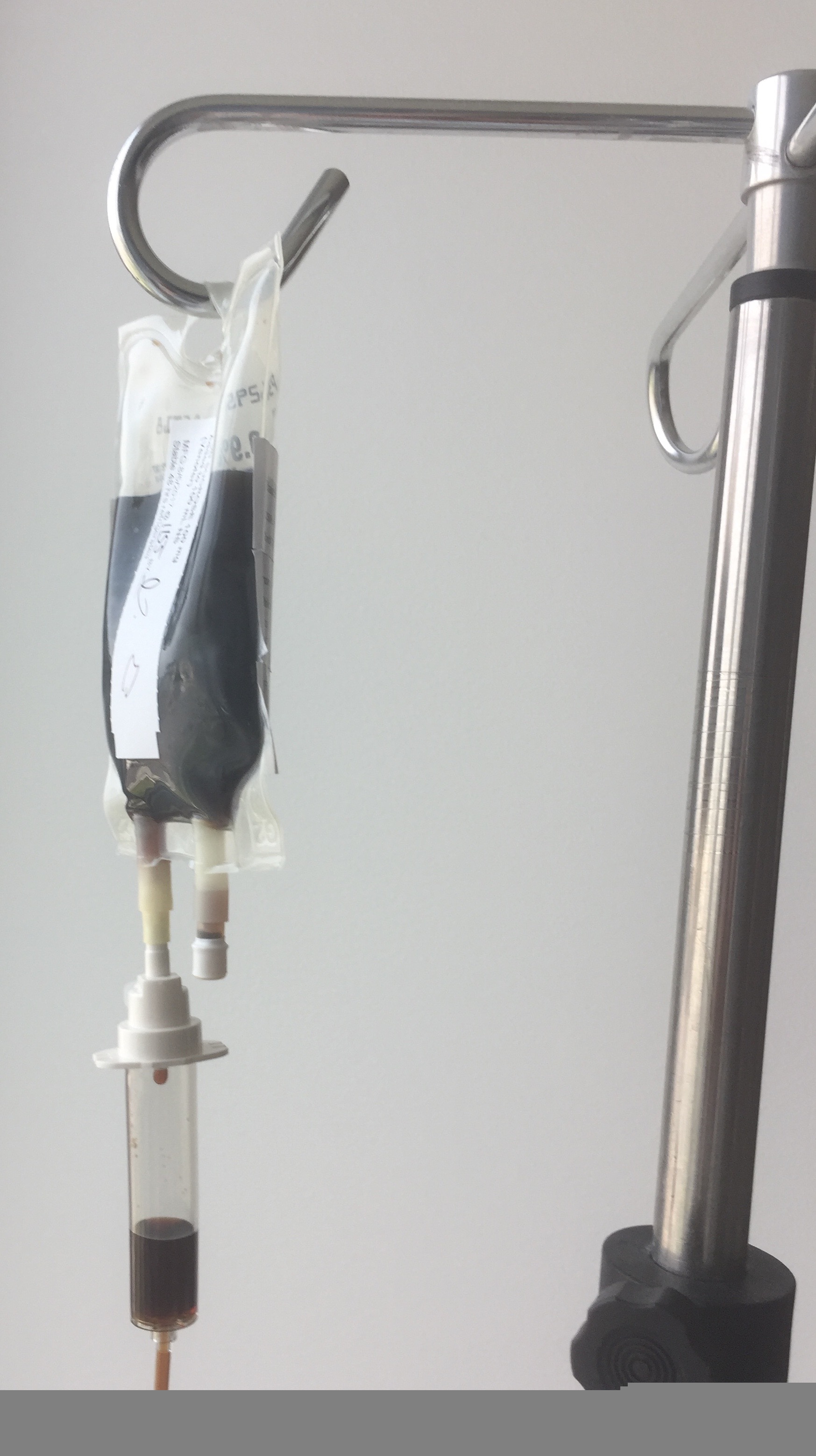
Children often receive the antibiotics through an intravenous drip (see images).
But colds, most sore throats and ear infections are caused by viruses and not bacteria, and antibiotic treatment is unnecessary and ineffective.
John Walley, Professor of International Public Health at the University of Leeds, said: “Doctors working in the primary care hospitals come under considerable pressure from parents to prescribe antibiotics to children who have upper respiratory tract infections.
“They can feel that if they don’t give the antibiotic, the parents will just go elsewhere and get it.
“These are difficult decisions for the doctor. They may have a very ill child in front of them – and they do not have a battery of tests results to rely on. They are having to make a clinical judgement about the risks involved in not giving antibiotics.”
University academics and Chinese experts drew up clinical guidelines based on those produced by the UK’s National Institute for Health and Care Excellence – to help doctors decide when it would be appropriate to prescribe antibiotics and alert them to the warning signs of more serious illness.
Two groups of primary-care hospitals in Guangxi were selected for the evaluation. Baseline measures were made of prescribing practices for children attending with upper respiratory tract infections.
In the first group – containing 12 hospitals – doctors received training in how to explain to parents why antibiotics are not necessary. Medical managers also conducted monthly prescription reviews, to monitor doctors’ compliance with the guidelines.
In the second group – made up of 13 hospitals – medical staff continued to prescribe in the usual way.
Six months later, several thousand prescriptions were selected at random from the two groups and compared with the baseline findings. The results showed that in the group that had received stewardship training, the antibiotic prescription rate had dropped from 82 per cent to 40 per cent. In the business-as-usual group, the rate went from 75 per cent to 70 per cent.
Taking account of statistical issues, the researchers say the training resulted in a 48 per cent reduction in the prescribing rate of antibiotics for children with upper respiratory tract infections.
Professor Walley said: “There have been other approaches that have tried to change the behaviour of doctors and patients – but none has delivered the scale of changes that we have seen.”
Typically in successful trials the change is between five and 25 per cent.
The Chinese Health Ministry has policies to reduce antibiotic use but the challenge is to get that aim delivered in primary care clinics and hospitals, Professor Walley said.
He said the key to success was to ’embed’ work within national policies and the health system, giving doctors the skills and encouragement to give antibiotics when there is a real clinical need.
The problem of the overuse of antibiotics exists in many low and middle income countries, and existed in the UK – although healthcare policies in recent decades have resulted in more careful use of antibiotics.




Leave a Reply