Bones, although composing the hardest tissue in the human body, are not stagnant structures. According to recent studies, bones maintain a lively metabolism and closely interact via nerves with the brain. But whether endocrine hormones also play an important role in brain-bone talk has been unclear.
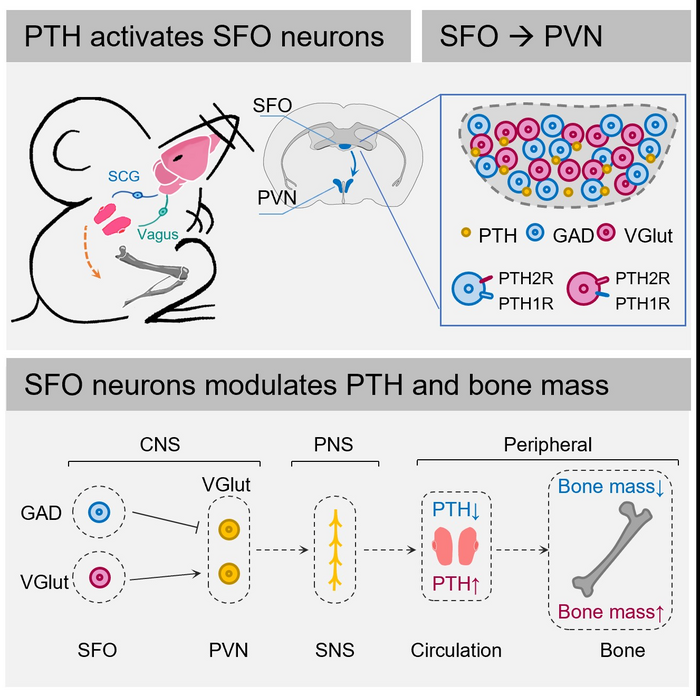
Researchers from the Shenzhen Institute of Advanced Technology (SIAT) of the Chinese Academy of Sciences now have an answer to this question. They have revealed that the subfornical organ (SFO), a brain nucleus above the third ventricle of the brain, senses circulating parathyroid hormone (PTH) and subsequently modulates the peripheral PTH level. PTH, as a powerful regulator of calcium and phosphate balance, may then alter bone metabolism and remodeling.
This study was published in Neuron on April 20.
If you enjoy the content we create and would like to support us, please consider becoming a patron on Patreon! By joining our community, you’ll gain access to exclusive perks such as early access to our latest content, behind-the-scenes updates, and the ability to submit questions and suggest topics for us to cover. Your support will enable us to continue creating high-quality content and reach a wider audience.
Join us on Patreon today and let’s work together to create more amazing content! https://www.patreon.com/ScientificInquirer
Using a mouse model, the researchers found that PTH from peripheral system bound to SFO, a circumventricular organ without a blood-brain barrier. Brain slice electrophysiology study and calcium fluorescent study indicated that peripheral PTH activated the SFO neurons.
The researchers identified the expression of PTH receptors on SFO neurons. Knockdown of PTH receptor 1 induced a decrease in basic PTH level in mice and their response to peripheral stimulation of calcium.
“These results indicate that the central nervous system (CNS) senses the circulating PTH, and the sensation of PTH from the brain is also necessary during the regulation of serum PTH,” said Prof. YANG Fan from SIAT, corresponding author of the study.
Furthermore, the researchers studied whether stimulation of the SFO neurons could modulate the peripheral PTH level in return. Both GABAergic and glutamatergic neurons were activated through chemogenetic technology. Stimulation of the inhibitory GABAergic neurons induced a decrease in serum PTH and a decrease in trabecular bone density, while stimulation of the excitatory glutamatergic neurons showed the opposite effect.
“What is worth noting is, GABAergic neurons dominate the SFO cells expressing PTH receptor 1 while the glutamatergic neurons dominate the cells expressing PTH receptor 2,” said Prof. YANG.
The research team also studied the brain nucleus downstream of SFO. They found that the paraventricular nucleus (PVN) of the hypothalamus that receives GABAergic projection from SFO also modulates the serum PTH level and trabecular bone metabolism.
Previous studies generally focused on the afferent and efferent nerve fibers surrounding bones when discussing brain-bone connections. Now the current researchers have revealed that chemical signaling through the endocrine system also plays an important role in brain-bone talk.
“Traditionally, the subfornical organ is taken as a center of water-salt balance. Our study indicates that SFO is far more than that. The loose blood-brain barrier structure in SFO endows it with a variety of abilities sensing the peripheral humoral hormones,” said Dr. ZHANG Lu, first author of the study. “We expect other circumventricular organs should also perform more in the interoception process.”
This study reveals the critical role of the brain-parathyroid-bone axis in maintaining bone metabolism homeostasis. It also provides new ideas for understanding how bone homeostasis is maintained.
IMAGE CREDIT: YANG Fan





Leave a Reply