An article published in the journal Frontiers in Cellular and Infection Microbiology reports a study by researchers at the State University of Campinas (UNICAMP) and the University of São Paulo (USP) in Brazil showing how a human protein interacts with a SARS-CoV-2 protein, and describing one of the ways the virus that causes COVID-19 recruits cells to replicate.
In laboratory tests, the researchers inhibited interaction between the molecules using a drug and thereby reduced viral replication by 15%-20%. They expect their findings to contribute to the development of treatments for COVID-19.
“The human protein known as PCNA [proliferating cell nuclear antigen] interacts with the SARS-CoV-2 protein M [matrix], one of the molecules that make up the virus’s membrane and give it shape. The discovery itself shows one of the ways the pathogen manipulates cell function for its life cycle to proceed,” said Fernando Moreira Simabuco, a professor at UNICAMP’s School of Applied Sciences (FCA) in Limeira and principal investigator for the study, which was supported by FAPESP.
HAVE YOUR SAY.
Join us in The Bullpen, where the members of the Scientific Inquirer community get to shape the site’s editorial decision making. We’ll be discussing people and companies to profile on the site. On Wednesday, July 20 at 5:30pm EST, join us on Discord and let’s build the best Scientific Inquirer possible.
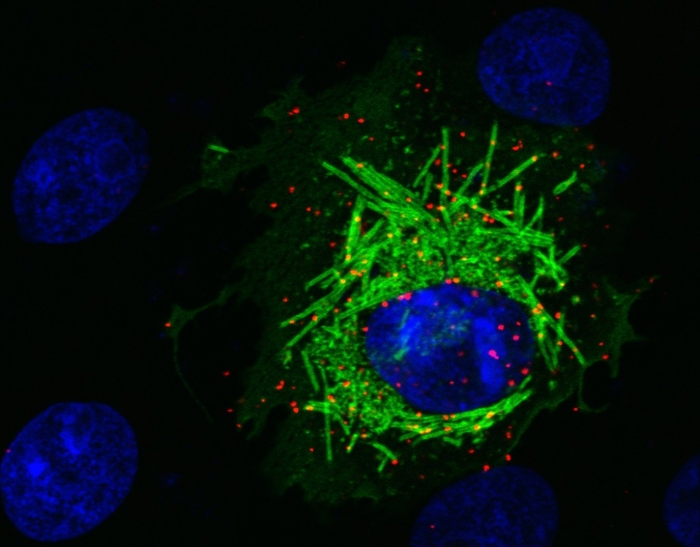
The group used a range of in vitro techniques to investigate how the presence of the viral protein M in the organism makes PCNA, a protein involved in DNA repair, migrate from the cell nucleus, where it is normally found, to the cytoplasm, a cellular region containing organelles responsible for important cell functions.
According to the researchers, this migration shows that the viral and human proteins interact, a conclusion corroborated by other methods, such as use of compounds to inhibit migration of proteins from the nucleus to the cytoplasm. In cells treated with both a specific compound for PCNA and another that inhibits migration of different proteins including PCNA, viral replication was reduced by between 15% and 20% compared with untreated cells.
“If we’d been thinking about treatment, perhaps this reduction wouldn’t have been significant, but our main aim was to demonstrate the interaction and show that it could be a future therapeutic target,” Simabuco said.
In collaboration with researchers in the Pathology Department of USP’s Medical School, they analyzed samples of lung tissue obtained during autopsies of deceased COVID-19 patients (more at: agencia.fapesp.br/32955/).
Expression of PCNA was found to be above normal in these samples, as was expression of the protein gamaH2AX, a marker of DNA damage, reinforcing the results.
“This finding may point to yet another consequence of infection by the virus,” Simabuco said.
The first author of the article is Érika Pereira Zambalde, a postdoctoral researcher at FCA-UNICAMP under Simabuco’s supervision.
Protein news
The protein M is anchored, with proteins E and S, in the membrane that envelops SARS-CoV-2, and is the most abundant of its four main structural proteins, called structural because they give it shape. For this reason, it has been considered a potential target for medications and vaccines.
S, the viral spike protein, is well-known because it binds to the ACE receptor in human cells, a role that has made it the target for most current COVID-19 vaccines.
The human protein PCNA is widely studied in the context of cancer research, as exemplified by a project conducted by Simabuco at FCA-UNICAMP. Little is known about the role of PCNA in viral infections, however.
The recently published article, therefore, offers a way forward for further research on this interaction between SARS-CoV-2 and PCNA, facilitating the development of therapies. A next step would be validation of the discoveries in animal models, although this has not yet been programmed.
Some of the experiments were conducted at the Laboratory of Emerging Virus Studies (LEVE) headed by José Luiz Proença Módena at UNICAMP’s Biology Institute (IB), with FAPESP’s support.
Research groups led by Armando Morais Ventura, a professor at USP’s Biomedical Sciences Institute (ICB), and Henrique Marques-Souza, a professor at IB-UNICAMP, collaborated in the study.
IMAGE CREDIT: Orlando B. Scudero/ICB-USP.




Leave a Reply